Gratitude Jonathan Byrnes, who joined the HBS Association of Northern California during the early weeks of the COVID crisis to educate the community on the topic of supply chain management. This topic is of imminent importance as it can help organizations improve access to needed resources while addressing the issue of organizational sustainability. This is extremely relevant to the distribution of PPE and other vital products and services today. Further, unless organizations manage quickly and carefully, their long-term viability is at-risk.
Interestingly, in the media, there has been a great deal of interest in his work because otherwise the conversation during the pandemic has centered on leadership vs management tactics, including supply chain. In his view, “There is little information regarding systematic, hands-on management in crisis.”

Jonathan is considered the creator of the field which we shared during his recent webinar, vendor-managed inventory, and has had extensive experience across industries, including health care, and geographies, including Indonesia. It was in Indonesia where he observed the country experiencing a supply chain shock not dissimilar to what we are experiencing today on a global basis.
It was fascinating to learn about Jonathan’s values and his career. He is driven by taking on new challenges, and therefore enjoys combining a career in academia, consulting, and profit analytics software. Through his work as a professor at MIT and as the principal of Profit Isle, a SaaS profit analytics company that has accelerated the profitability of over $100 billion in client revenue, he has worked with thought-leaders, like Ben Shapiro, Malcolm P. McNair Professor of Marketing, Emeritus at HBS, among others, to create important innovations in his field. These have resulted in important improvements both on how customers get access to the products they need, and on business profitability and sustainability.
Highlights of his presentation included observations on the tendency of organizations to use inefficient models for profitability assessment. Specifically, he pointed out that there are customers that either augment or drain profits and that businesses should focus on serving the customers that generate the most profits and spend fewer resources on unprofitable ones. This goes against the more common but far more destructive tendency to service them all.
Additionally, we learned that there are certain “secret weapons” during crises like these, including (1) substitutions (he cited Dell as an example), as well as (2) preventing over-ordering, which involves both addressing the tendency to over-order and to over-produce. It was interesting to learn that most of the supply chain disruptions we are reading about today could have been prevented with expert management.
To learn more about Jonathan Byrnes and his recommendations regarding supply chain management during the crisis, we encourage HBS Association of Northern California members to view his webinar and to read , Coronavirus: Five Rules for Growing Customer Loyalty.







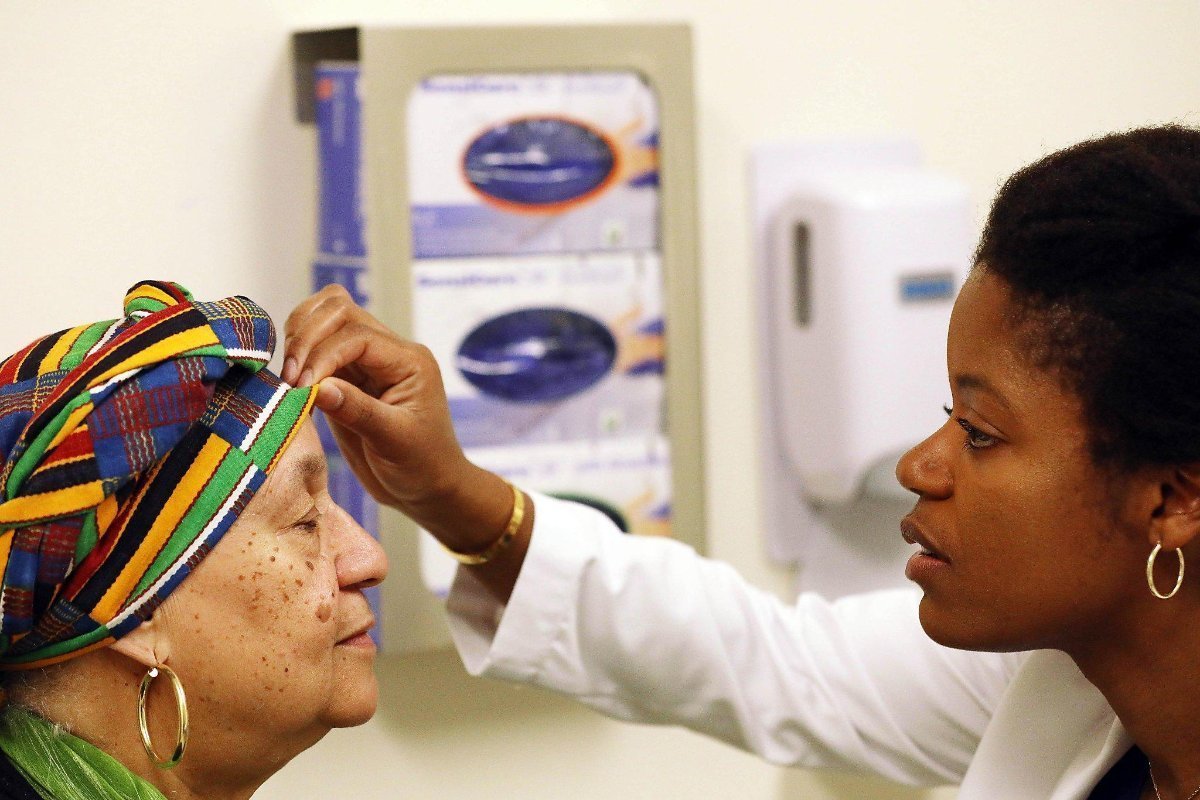 The piece reveals, “Dr. Jenna Lester may be the only black dermatologist in San Francisco”.
The piece reveals, “Dr. Jenna Lester may be the only black dermatologist in San Francisco”.


